A recent measles outbreak traced to Disneyland has put anti-vaccination advocates under the microscope once more. With upwards of 80 people now diagnosed with measles, it’s worth asking why this preventable disease has again been allowed to endanger public health.
According to The Los Angeles Times, only seven of the 39 patients whose vaccination status is known were fully vaccinated at the time of the outbreak. The numbers are not surprising. We know now that anti-vaccination parents tend to live in clusters, grouping in particular states and, in the case of California, particularly affluent parts of the Bay Area. This map from the Centers for Disease Control highlights states with higher vaccination exemption rates in darker shades of blue, and fewer vaccination exemption rates in lighter shades:
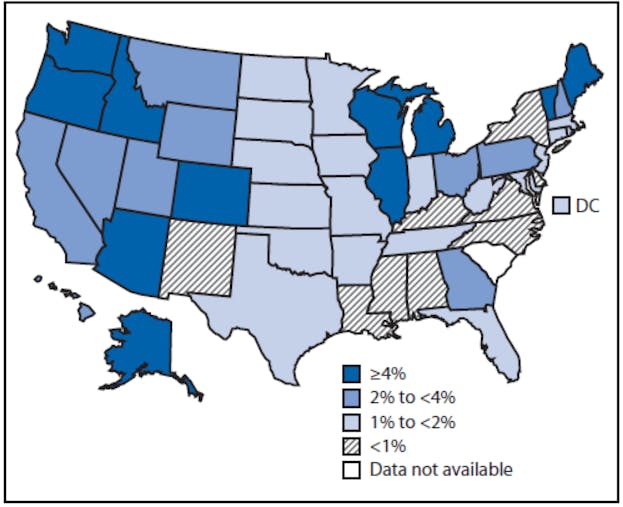
The clustering of anti-vaccination types around certain geographic pinpoints—especially the Pacific Northwest—may suggest that vaccine denial is tied up in subversive, countercultural sentiment. But compare research on Americans who resist vaccination and Swedes who willingly sign up for optional vaccines, and it seems as though anti-vaccination advocates are the most American of us all.
Consider sociologist Jennifer A. Reich’s 2014 article "Neoliberal Mothering and Vaccine Refusal: Imagined Gated Communities and the Privilege of Choice," published in the journal Gender & Society. Reich researched women who advocate against and refuse vaccines, and the techniques they use to obtain legal exemptions from them. Reich concludes that the well-off moms who skip out on vaccines do so...
…by mobilizing their privilege in the symbolic gated communities in which they live and parent. They utilize resources that facilitate their choices as informed consumers without feeling compelled to support the health or decision making of other families with fewer resources. They also refuse to acknowledge the role their children play in protecting or undermining systems of public health...
In other words, parents who opt out of vaccines come to their decisions by prioritizing the very virtues American culture readily recommends: freedom of choice, consumer primacy, individualism, self-determination, and a dim, almost cynical view of common goods like public health. If enclaves of anti-vaccination advocates are limited to the rarefied exurbs of California and Oregon, then the prevalence of this "neoliberal" frame makes all the more sense, as a certain laissez-faire attitude toward matters of mass coordination is associated with wealth and an attendant sense of personal control: Since money affords the wealthy a certain amount of control over their personal affairs, they both experience feelings of control (which may or may not correspond to reality) and feel less concerned with the welfare of others. After all, if one is convinced they can manage their own affairs, why shouldn't everyone else be able to?
Compare Reich’s data with a similar study published in The Scandinavian Journal of Public Health circa 2013. Conducted by Swedish political science scholar Björn Rönnerstrand, the study sought to understand differences between Swedes who chose to be vaccinated against the H1N1 virus in 2009 and those who did not. Rönnerstrand controlled for a number of factors, including age, sex, gender, education, and even level of concern about an H1N1 pandemic, meaning that the decision to be vaccinated or not couldn’t be confounded by, say, a person’s individual panic level or knowledge of infectious disease.
So what separated Swedes who sought vaccination and those who didn’t? Rönnerstrand found that those who sought vaccinations had high levels of institutional trust—that is, trust in the Swedish healthcare system—and high levels of generalized trust, or trust in the rest of society. Rönnerstrand notes that in “a promotion campaign during the 2009 (H1N1) pandemic, the Swedish Institute for Communicable Disease Control emphasised that individual immunisation—besides strengthening individual protection—was a way of protecting fellow citizens,” and suspects that this had a major impact on general willingness to be vaccinated. “It is well known,” he goes on, “that Sweden belongs to a group of northern European countries where citizens have high trust in institutions as well as in fellow citizens.” In other words, along with a healthcare system they can rely upon, Swedes are inclined to care about and protect one another, and feel secure that others feel the same about them.
This ethic is, of course, quite contrary to the American fantasy of rugged individualism, which functions in a feedback loop with American politics: culture influences politics, and laws and political rhetoric in turn influence culture. While conservatives daydream about an American idyll of self-sufficiency and liberty, the new House GOP is set to hold its first repeal vote on the Affordable Care Act, the closest thing to a unified healthcare system the United States has ever known. The idea that everyone should ultimately be individually responsible for her own health directly animates the idea that there need be no unified, reliable healthcare system—and those two ideas preclude anything approaching Sweden's trust in healthcare or society at large. Individualism begets individualist politics, both of which encourage the type of thinking anti-vaccination advocates appear prone to.
It’s all well and good to roast anti-vaccination sorts in the media, and it isn’t as though they don’t deserve the righteous condemnation of the masses they put at risk when they allow once-defeated diseases to return. But to extinguish large swathes of anti-vaccination sentiment and practice, it appears a more momentous cultural shift is in order, and a pursuant political change. Trust requires mass coordination of efforts, which in turn requires consistent trust—something neoliberal politics in America vastly undervalues. To prevent future outbreaks, we should try to be more like the Swedish.
