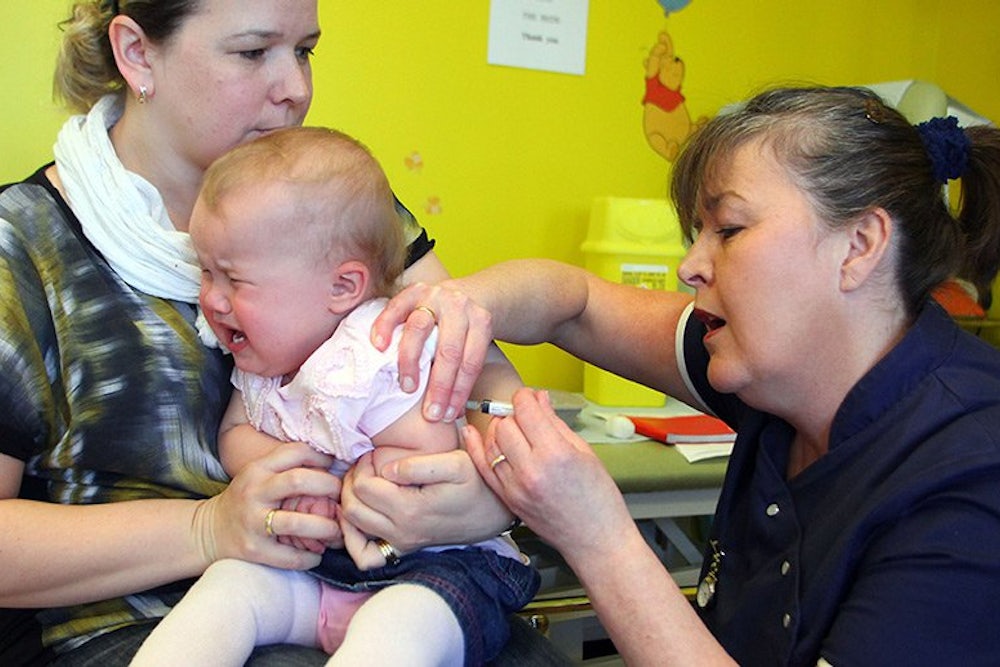
As the measles outbreak sparked at Disneyland continues to spread, the debate about so-called anti-vaxxers and individual rights has taken on a political valence, with Chris Christie and Rand Paul remarking skeptically on vaccines and President Obama coming out strongly in favor. And yet, watching the cultural tug-o-war over vaccines degenerate into a partisan skirmish, a few distinctions are necessary.
Anti-vaxxers are a tiny community of diehard opponents to vaccination who live in geographically dispersed enclaves throughout the country. These are the people who hold fast to nightmare stories about a causal link between autism and vaccines, who argue that infectious disease can be prevented with old-fashioned diets, who spread conspiracy theories about scientists whose work shows that vaccines are perfectly safe. They are a relatively obscure and minor set, rarely drifting to the fore of public debate unless there is an outbreak of illness at hand.
Though perhaps willing to court their vote, I doubt Christie or any member of the Republican mainstream lines up with genuine anti-vaxxer sentiment. On the other hand, when not spouting incoherent and directly refutable nonsense, the anti-vaxxer crowd has one appeal that strikes a chord with the American right wing: an objection to the fact that many vaccines are mandatory, that is, required by state mandate. The idea that parents should be presented with options rather than mandates was, after all, the real substance of Christie’s statement, though perhaps cynically timed.
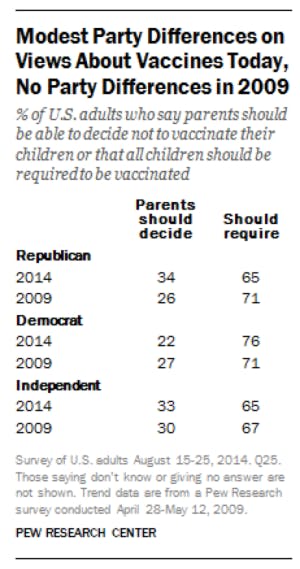
So perhaps we should consider splitting up the two simultaneous arguments at hand: first, are vaccines efficacious, and do they represent a public good? Indisputably. Must vaccination be mandatory in order to achieve the protection of the masses, especially the most vulnerable?
That’s a more difficult question.
Herd immunity, or mass community immunity to particular illnesses, is the goal of vaccination. Different diseases have different thresholds for herd immunity, depending on how contagious they are. For measles, a highly contagious disease, the threshold for herd immunity is 95 percent community immunity. For diseases less contagious, like polio, the threshold may be ten to fifteen percent points lower. Though overall rates of childhood vaccination coverage in the United States remains high, the fact that groups who resist vaccines in higher numbers tend to cluster together means that there are pockets of vulnerability strewn throughout the country that are a threat to people who cannot be immunized due to age or illness.
In light of this, some have suggested doubling down on vaccine mandates by attaching additional penalties, legal and otherwise. There have been calls for an end to religious and personal exemptions for vaccines, which currently allow unvaccinated children admission to public schools. Others have suggested suing or criminally charging parents who choose not to vaccinate their kids. More yet have praised pediatricians who have elected not to treat unvaccinated children in order to protect other patients in their offices.
But it doesn’t have to be this way.
In a variety of European countries, including the United Kingdom, Sweden, The Netherlands, Norway, Denmark, and Finland, high vaccination coverage (up to 99 percent in Finland, for example) has been achieved without the use of mandates. Is this a possible third way for Americans, dissenting to anti-vaxxer sentiment while still avoiding a direction that penalizes parents and children without making the rest of us much safer?
In short: it could be, save for what the American objection to mandates represents. Insofar as we detest mandates because they are an affront to our self-sovereignty, it seems unlikely that removing mandates and encouraging vaccination through voluntary means would do much to improve the willingness of fiercely individualistic Americans to risk their health or comfort for the good of the whole society. As Michael Gerson once wrote of capitalism, a mandate-free vaccination regime enacted strictly out of American disdain for obligation would rely on virtues it would not create.
But there’s another hitch. As researchers from a number of European universities wrote in the scientific journal Eurosurveillance, “a national healthcare system should promote and actively offer those vaccines that have been proven to be safe, effective, and with a positive public health impact. In a world where people trust health authorities, more compliance with national recommendations can be established.” In other words, the creation of a healthcare system that is both accessible and trustworthy is a key factor in ensuring widespread voluntary vaccination. This is true not only because a universally accessible healthcare system would make vaccines readily available to all people, but also because frustration with expensive and unreliable healthcare contributes to the kind of mistrust that makes people suspicious of vaccines themselves.
Of course, pernicious American individualism is as much an enemy of a trustworthy universal healthcare system as it is of voluntary mass vaccination. Rand Paul once excoriated the idea of universal healthcare by equating such systems with forced labor. “With regard to the idea of whether you have a right to health care,” Paul claimed in a 2011 meeting of the Senate Committee on Health, Labor, and Education, “you have [to] realize what that implies. It’s not an abstraction. I’m a physician. That means you have a right to come to my house and conscript me. It means you believe in slavery.”
In no universal healthcare model are doctors forced to perform labor for free, but the revealing fact of Paul’s statement is that it all comes down to him, personally, and his personal freedom. This is the recurring priority of American politics, and the one that makes high vaccination coverage in a non-mandatory scenario seem a distant proposition. Vaccines are, contrary to popular thought, ultimately a matter of collective action, and one that comes down mostly to thoroughgoing altruism. Unless we can manage to leave self-interest on the back burner and pull together in favor of our society’s most vulnerable people mainly for their own sake, we will likely never create a political climate that can ensure both safety and freedom in the realm of disease.