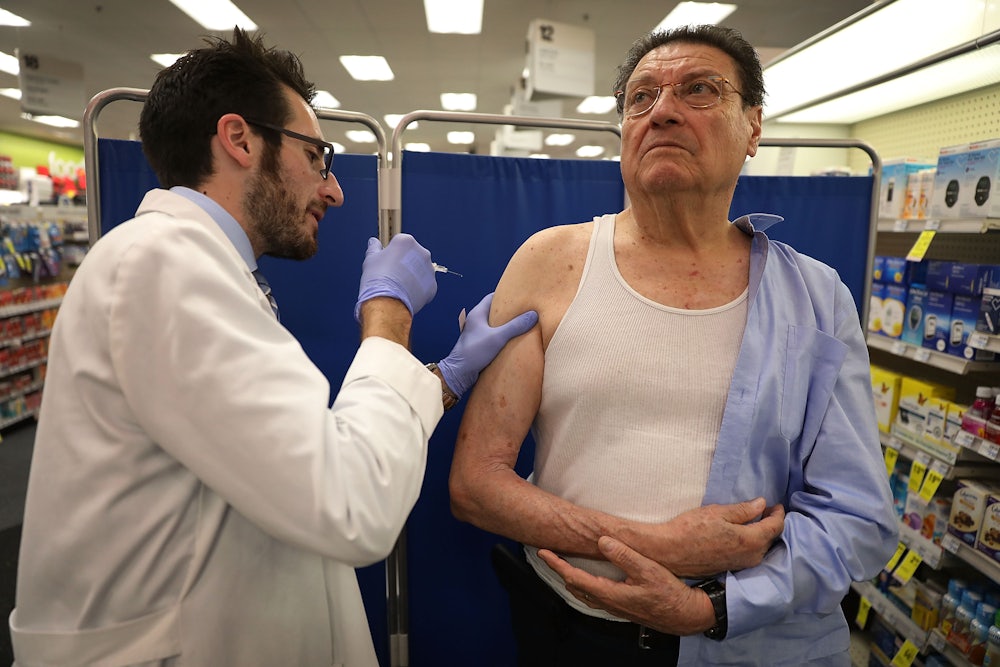
It’s not certain that we’ll ever get a vaccine for the coronavirus, let alone that one will be available by January, as Anthony Fauci has suggested as a hopeful possibility. As Alexander Zaitchik wrote for The New Republic, the pharmaceutical industry’s greed has devastated America’s ability to produce new vaccines. In fact, he argues, the manufacturing of anything that might not be profitable may be no longer within the industry’s grasp. Our unique dedication to letting the market decimate whatever it desires will not be limited to the process of discovering a vaccine, however: It will hamper our ability to distribute it, too.
The dissemination and administration of a coronavirus vaccine is a global task, and there is a great risk that the same pattern of false scarcity and profiteering that plagues the availability of pharmaceuticals will hamper any such effort. It is worryingly likely that the United States and other rich countries will get access to the vaccine first simply because their patients, or their governments, are willing and able to pay more than poor countries. But even within the U.S., it will be difficult to distribute the vaccine equitably.
The U.S. simply does not have anything resembling the infrastructure necessary to ensure that everyone gets anything, including food or water or shelter, let alone something that requires access to a health care worker. To the extent that we have ever aspired to this sort of capability, those traditions have long eroded, worn down by our debased politics. We do not have a National Health Service–style system, which was able to produce a (poorly handled but nevertheless extant) list of patients who were at high risk for the coronavirus. My mother in Britain, who has received immunotherapy for lung cancer for the past two years, was on this list. She received a text from the government telling her to stay inside for 12 weeks, plus a phone call and two letters, which also advised her of government resources for food and help for the extremely vulnerable and suggested that she spend time with the windows open or sitting on her doorstep.
Where is such a list in the U.S.? The task of administering an eventual vaccine and ensuring everyone has received it will likely be put to the thousands of independently run doctors’ offices, many of which are already at risk of closure, and pharmacies. The companies that thought Theranos was the future might be leading our battle for herd immunity. You will be sold a Twix and a Gatorade with your coronavirus vaccine: lucky, then, that your diabetes will no longer put you at higher risk of dying of Covid-19. Welcome to America.
Vaccinations pose a challenge in the best of times. For example, a majority of Americans do not receive a flu shot each year. There are many reasons for this, including misconceptions about how it works and why it’s necessary. A 2012 study of flu shot uptake in a low-income community in New York reported that of the participants who intended to get the shot but hadn’t yet, 95 percent said the reason was that it was difficult to access the vaccine. Fewer poor people get the flu shot overall, and more poor people die of flu. Understandable distrust of the medical profession by poorer individuals—let alone members of the thoroughly more bourgeois anti-vax movement, who are sure to decide that the coronavirus vaccine causes autism, too—might well pose a challenge to administering the vaccine. The one thing we have going for us, where rolling out a nationwide effort to vaccinate the populace is concerned, is that the coronavirus is at least a very visible problem. You can be pretty sure that everyone has noticed the economy has stopped, and that the vast majority of people will be eager to get back to normal.
Yet it seems impossible that a coronavirus vaccine would turn out to be the only thing that is not more easily accessible to the rich in the U.S. The megawealthy, after all, immediately finagled access to coronavirus testing, while populations at greater risk of infection continue to wait for a testing infrastructure beyond its current threadbare state to be spun up. It’s hard to imagine that some Silicon Valley company named Elixir or PlasMa won’t end up with early stocks of the vaccine. It’s similarly difficult to shake the notion that fault lines won’t just be drawn between multimillionaire 0.1 percenters and the rest of us, but between ordinarily wealthy people and the struggling poor. You only have to look at the scores of people who turn up for Remote Area Medical clinics to imagine the difficulty we may have.
America does not really have a health care “system” at all; it has a chaotic array of overlapping systems of private and public health financing, clinics, hospitals, and doctors. This lack of a single system will pose a challenge for administering a vaccine to the entire population. It’s not as simple as adding one more to the list of vaccines that children receive or distributing vaccinations at schools: People of all ages will need one. Can you name a physical institution that every American interacts with and has easy access to and that is prepared to distribute something universal like this? The Social Security office? The DMV? McDonald’s? (Starbucks and McDonald’s bathrooms are often the only place homeless people can go to freshen up, so it’s not like we’re not used to substituting chain restaurants for a society.) The closest thing might be the post office, currently in danger of being left to rot and die because of the virus. It may be that setting up post offices with government-employed pharmacists to distribute the vaccine would be our best bet, given the lack of universal access to medical settings.
It is far from guaranteed that an eventual vaccine will be made available free of charge. In this week’s Senate hearing on the coronavirus pandemic, health officials declined to say that the vaccine would be free. Dr. Brett Giroir, who currently serves as the assistant secretary for health in the Trump administration, went only as far as suggesting that the poor “should have access to it.” (To quote Malcolm Tucker, “should” does not mean “yes.”) Given the fact that the president believes that the second Iraq War should be paid for with plundered Iraqi oil, no one should be under any delusion that Trump will easily give up the prospect of allowing someone to profit from a vaccine. But even if we imagine that an eventual vaccine might be required by a more benevolent future Congress or administration to be issued for free, the health financing system we have has already eaten away at our ability to distribute a vaccine on a universal scale.
In 2015, just 75 percent of Americans had a regular primary care physician. This is partly due to shortages. The U.S. has about half as many primary care doctors as other countries and far more specialists, who are paid far more in this country than elsewhere: It is simply much more lucrative for doctors to become knee surgeons or dermatologists than family doctors, so that is what they do. The shortage is much worse in poorer neighborhoods: According to an investigation by The Pittsburgh Post-Gazette and The Milwaukee Journal Sentinel, 58 percent of locales federally designated as “primary care shortage areas” are in high-poverty areas. The prevalence of disabled residents is higher in those places, and the rate of premature deaths is 39 percent higher in poor counties. Yet, the investigation found, rich areas are the ones getting new hospitals. This is an inevitable consequence of a health financing system that is formed around squeezing money out of fat private insurers—or, if you prefer, a system that champions profit-taking over provision.
Poorer hospitals that provide care to underserved populations are already at greater risk of closure because of the loss of more lucrative elective procedures. If the coronavirus pandemic threatens this revenue stream for months more—and particularly if the premature “reopening” of the economy causes a resurgence of Covid-19 cases, a cycle that America is easily dumb enough to repeat multiple times—those hospitals will be the first to collapse. The same goes for health clinics, those places that currently serve as the first or only source of care for many poor Americans. In a world even marginally more sensible, those clinics would be perfect places to distribute vaccines to the poor; instead, they might fold before they have the chance to try.
Since some vaccines, like the flu shot, are simple enough to administer at pharmacies, it seems likely that a coronavirus vaccine could end up being distributed through your local CVS. But access to pharmacies is limited for poorer areas, too. A 2014 study of pharmacy access in Chicago, published in Health Affairs, found that “pharmacy deserts” plague poorer communities, particularly segregated black and Hispanic communities. This is especially concerning given that the virus is killing more black and Hispanic people. Rural areas, too, are suffering from a decline in pharmacies. A study by the RUPRI Center for Rural Health Policy Analysis found that 630 rural communities that had at least one pharmacy in March 2003 had none by March 2018; the Center’s director told US News and World Report that “a pharmacy located as far away as 30 or 40 miles might do once-a-week or twice-a-week deliveries in the community” in some areas, with others turned to telehealth. As wonderful as modern technology is, it is not currently possible to administer a vaccine over the internet.
This is the hollowing out of America. Institutions that serve the poor are being squeezed and shuttered, while options for the comfort and happiness of the rich grow by the day. A glossy shell may remain, but what’s inside has been eaten away, leaving the whole thing far more fragile. The well-off may come to regret this state of affairs, profitable and pleasant as it has been for them, when it comes time to achieve herd immunity from the coronavirus. If we need to vaccinate 85 percent of the population to do this, the rich will have to hope that not more than 15 percent of the country is disconnected, disenfranchised, and dispossessed, unable to access or afford the vaccine. Good luck with that.