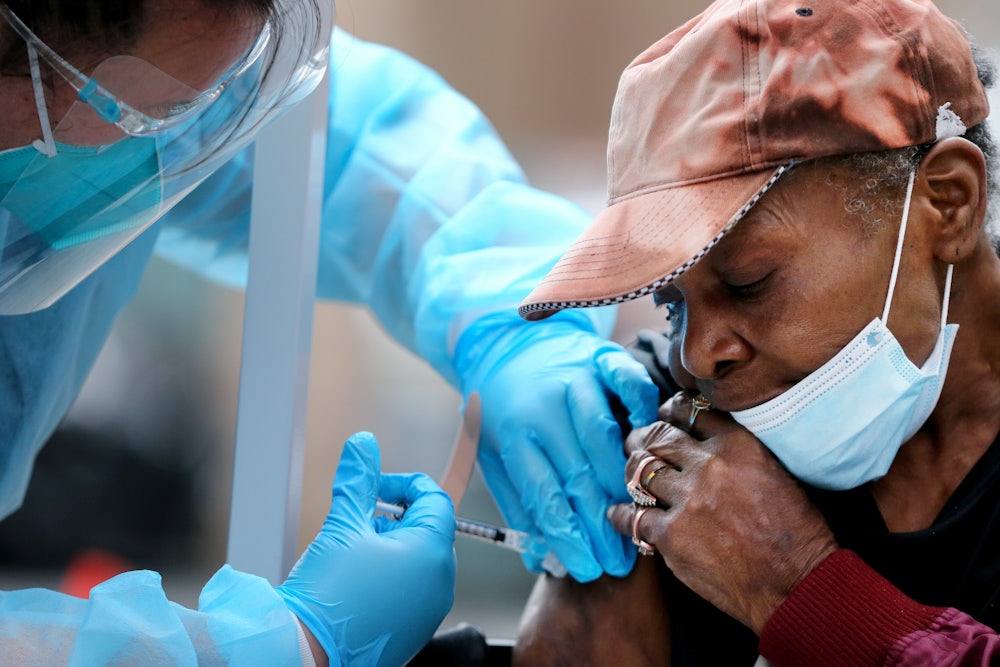
Dr. Oni Blackstock finished seeing patients one day in late December, and then she became the patient for a few minutes: She rolled up her sleeve and got her first Covid-19 shot. But as she chatted with the nurses—both at work that day and while filling out paperwork for the vaccine—she encountered the same line from several of them: “I’d like to wait and see.” While some of the nurses were clamoring to receive their own vaccines, others were wary.
It may be surprising to hear that even health workers, who have worked tirelessly to combat the pandemic over the past year, have questions about the safety and efficacy of the Covid-19 vaccines. One national survey found that 15 percent of health workers choose not to get one—for now.
But that’s understandable, said Blackstock, who is a primary care and HIV physician and a former assistant commissioner at the New York City health department, especially because there was little education or outreach to health workers before the vaccines began rolling out. Answering questions about them—like whether you still need a shot after having Covid-19 (yes)—is as important as nailing the distribution of the vaccine, experts said. “Yes, it seems like it was developed really quickly, yes, I could understand your concern about that,” Blackstock told me. “And then you can ask permission to say, ‘Can I share some information with you that you may not be aware of, or that might be helpful in your understanding of the vaccine?’”
The Covid vaccines are a marvel of science, a “triumph”—incredibly safe, overwhelmingly effective, and, in the United States, expected to be available to anyone who wants them by this summer. But there’s the rub: anyone who wants them. The next challenge of the pandemic isn’t scientific or medical; it’s personal. Will enough people get vaccinated to bring the pandemic to heel?
Addressing this challenge can be as straightforward as listening, understanding, and responding to concerns, experts say. And that response is as simple as this: The vaccines can save your life and the lives of everyone you love. They will be a critical tool for ending the pandemic.
There are varied reasons for vaccine hesitancy, which is a global problem, ranging from concerns about how quickly the vaccines were created to politicization of the process to mistrust in the scientific and medical establishment.
Trump made rapid vaccine approval a centerpiece of the latter months of his presidency and his failed reelection campaign. With every boast of speeding up the process, public confidence in the vaccine dipped. However, regulatory agencies like the U.S. Food and Drug Administration stood firm and evaluated the vaccines without succumbing to political pressure. “The vaccine development process has gone very, very well, and it’s been done with great scientific integrity,” Dr. Ashish Jha, dean of the Brown University School of Public Health, told me.
Since Joe Biden’s election, more people are reporting an eagerness to become vaccinated. In December, 60 percent of Americans said they would get a vaccine when it became available, up from 51 percent a few months before, according to a Pew Research Center poll. A recent report from the nonpartisan Kaiser Family Foundation found that 41 percent of Americans would get a vaccine immediately, with 31 percent saying they want to wait and see, and only 13 percent saying they would refuse the vaccine. Yet another poll from the Associated Press-NORC Center for Public Affairs Research showed that two-thirds of Americans have already been vaccinated or plan to do so, while one-third probably or definitely wouldn’t. On Wednesday, The Lancet announced a new commission on vaccine refusal, acceptance, and demand in the U.S. in order to understand these concerns and how they could affect the course of the pandemic.
Why do these numbers matter so much? Reaching herd immunity—the point at which unvaccinated people are still protected against a virus by a circle of vaccinated people—would require about 75 to 90 percent of people becoming vaccinated, which may not happen even when enough shots are available. (The herd immunity estimates for Covid-19 have gone up in light of variants that may evolve to become more transmissible, even with vaccines.) But it’s not all or nothing. The more people are vaccinated, the more protected we will all be, even if we don’t eliminate the virus entirely (which, given the global nature of the outbreak, experts don’t expect to happen for years, if ever).
Having open, supportive conversations may be the best way to make sure our friends and family are protected by vaccines. Focusing on how effective the vaccines are, how well they protect us from illness and death, and the potential they offer for returning quickly to normal life are the most effective strategies for changing opinions on vaccines, research shows.
The problem of persuasion is not as daunting as some headlines suggest. Hard-line anti-vaxxers—those who reject all vaccines—represent only a fraction of the population, while nearly 20 percent of parents have some hesitation about vaccines. But having questions about Covid vaccines is not the same as being anti-vax or even vaccine-hesitant.
“This is not the run-of-the-mill vaccine hesitancy,” Dr. Saad Omer, director of the Yale Institute for Global Health, told me. Instead, the one-third of people who aren’t sure if they would take a vaccine today simply want to learn more about the science, safety, and side effects before making a decision. You might call it “vaccine thoughtfulness” instead. And this “short-term hesitancy is not the same as long-term refusal,” as Dr. Brian Wasik, a research associate at Cornell University, has pointed out.
The majority of people who haven’t made up their minds yet usually get vaccines, Jha said. They just want to do their due diligence on these shots because of the unusual circumstances around them. “My approach on this is to speak to people openly and plainly and share with them that the vaccines have all gone through all the checks and all the safety checks we would do,” Jha said.
Dr. John Moore, professor of microbiology and immunology at Weill Cornell Medical College, understands that some people are worried about potential side effects. “But here’s the thing: Everything is a balance. There’s a substantial risk of people dying of Covid, and that’s a real, apparent, present danger now. So you have to balance that against a low, and possibly nonexistent, risk of rare events occurring for the vaccine recipient,” he said. And part of the hesitations around safety have to do with flawed risk analysis. “Across society, people’s assessment of risk is often just way off the mark,” he said. “There’s a very small risk of a vaccine side effect. There’s a very significant risk of getting and dying of Covid.”
For some communities—particularly communities of color—questions about the vaccine often go deeper, to centuries of medical marginalization and abuse. “Black Americans remember Tuskegee. Hispanic Americans may fear harassment by ICE,” Dr. Jerome Adams, surgeon general of the U.S., has said. On Friday, President Biden toured the Pfizer manufacturing site in Michigan and said in a speech, “We all know there’s a history in this country of having subjected certain communities to terrible medical abuses in the past. But if there’s one message to cut through to everyone in this country, it’s this: The vaccines are safe.”
A new national survey found that initial skepticism about the vaccines in communities of color has been replaced with widespread acceptance. For instance, while 35 percent of Black Americans said in November they would get the vaccine if offered, that rate shot up to 59 percent in February. This is in marked contrast to other groups, such as one-third of white Republicans who have consistently rejected the vaccine.
Rather than medical mistrust, the major issue facing communities of color is a lack of access to vaccinations—the time off work needed to book and attend appointments; information on why, how, and where to get vaccinated; appointments in their neighborhoods that aren’t snatched up by others. Across the country, the vaccine rollout has been appallingly unequal, with white Americans taking vaccination slots two or three times more than Black and Hispanic Americans. Many people don’t know how or where to get the vaccine—but that knowledge gap is wider in communities of color, research shows. Bodega owners in New York, for example, have been eligible for shots since January 11, but many didn’t know that.
Acknowledging the racism and discrimination in health systems—both historical and current—is key for overcoming inequity, Blackstock said. And leaders in the community, from pastors to radio DJs, can be among the most effective voices on vaccine information, she said. “Particularly for groups that are marginalized and oppressed … the trusted messengers are really vital. Having folks that not just look like you but that are from your family, your community, your social network, is incredibly important.” As Jha puts it: “The messenger is as important as the message.”
That’s part of why Blackstock takes the time to ask nurses and other health workers what they’re thinking. These conversations don’t just benefit the health workers. Many patients feel more comfortable chatting with nurses and front-desk staff than with their doctors—asking what they really think or if they’ve gotten the vaccine themselves. Conversations like these could be an excellent way to help inform patients about the importance and benefits of the vaccines, Blackstock said.
As more people receive the Covid-19 vaccines, others will be reassured about their safety and effectiveness, experts say. “People are going to watch their friends and their family and their leaders get vaccinated. And they’ll see that people do well,” Jha said. “I’m pretty confident that the majority of Americans will end up getting vaccinated.” He paused. “Because who does not want to put this behind us?”