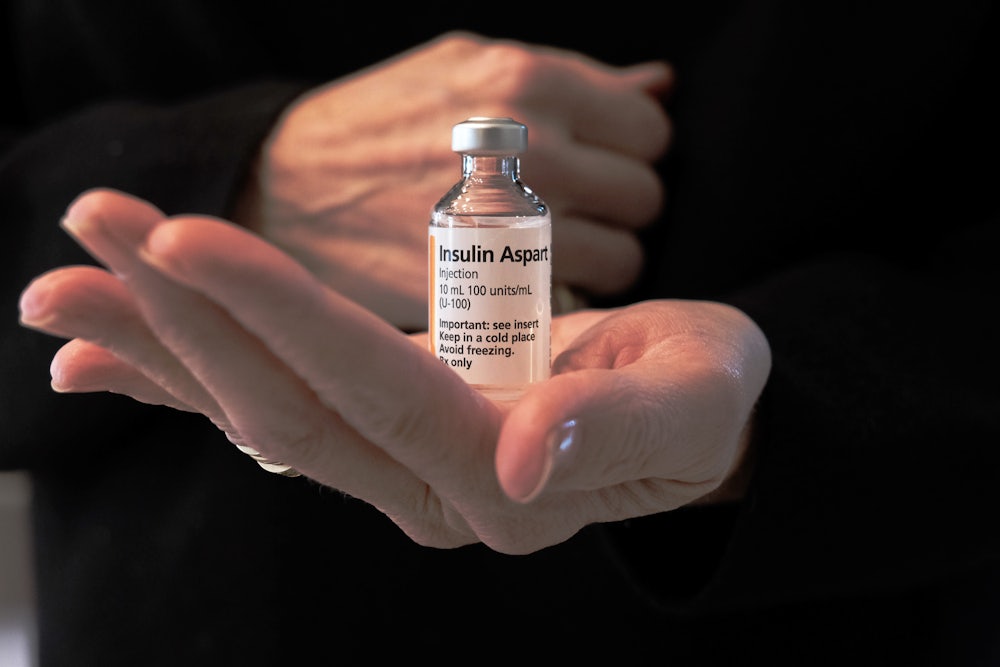
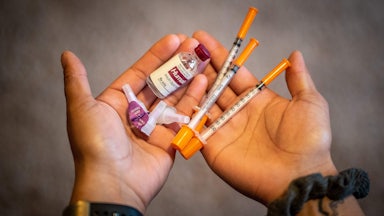
On Wednesday the pharmaceutical company Eli Lilly announced it would significantly lower the list price of some of its most common insulin products and cap the out-of-pocket patient costs to $35 per month. The decision to lower prices follows years of advocacy and political pressure to make insulin more affordable. Although the manufacturing costs of insulin have remained mostly the same, the cost of the four most commonly used types of insulin has tripled in the last decade, resulting in roughly one in four diabetics reporting rationing their insulin because of cost.
On the surface, Eli Lilly’s announcement is wonderful news to the millions of patients who are reliant on its medicine. But while the decision is bound to give Eli Lilly a fresh round of good P.R., its decision to lower prices obscures the reality that access to lifesaving medicine should have never been left up to the whims of a pharmaceutical company in the first place. Prices that go down today, after all, could go back up again tomorrow, and patients paying hundreds of dollars a month for insulin pens—including those in the expanded customer base Eli Lilly will build as a result of the price cut—deserve a guarantee that their costs will not rise at some point in the future because of new decisions made by whoever happens to be running the show at a private company.
Insulin, in particular, has become a political lightning rod over the past few years for a myriad of reasons. One is the sheer number of Americans who suffer from diabetes: According to the Centers for Disease Control and Prevention, roughly 32 million Americans are diabetic and another 90 million are prediabetic, meaning their blood sugar levels show they are at a heightened risk for developing the disease. Diabetes is considered the most expensive chronic illness, with $1 out of every $4 spent on health care going to the condition.
But the biggest reason that diabetes has become a hot-button political issue is that the cost of insulin provides a textbook case study of everything that is wrong with the American health care system.
Insulin was invented over 100 years ago, and the researchers sold the patent to the University of Toronto for $1 each. At the time of the sale, the chief scientist noted, “Insulin does not belong to me, it belongs to the world.” The rights were then sold to Eli Lilly and Co. so that the company could mass-produce the medicine. Over the past century, Eli Lilly—along with Novo Nordisk and Sanofi, who together manufacture 90 percent of the world’s insulin—have raised prices continuously.
In 1996, Humalog, an insulin developed by Eli Lilly, sold for $21 for a month’s supply. By 2019, the cost had risen 1,200 percent to $275 per month. In 2021, the drug company announced it would reduce the price of its generic version of Humalog to $137 for an individual vial, down from $275. This was welcome news, but Eli Lilly sold the same insulin to Germans at an even lower price of $55 for a vial. That same year Humalog was Eli Lilly’s bestselling drug, raking in $2.7 billion in sales. As part of Wednesday’s announcement, the company said it would lower the list price even further in the United States to $66, but this is still more than the average $43 it charges insurance companies after rebates.
Presidents Joe Biden and Donald Trump both made efforts to lower insulin prices; each met with fierce resistance from the pharmaceutical lobby. Trump attempted to lower Medicare costs by requiring drug companies to charge “most favored nation” prices. What Trump failed to realize is that other nations pay five to 10 times less for insulin because their governments are not prohibited from bargaining directly with pharmaceutical companies over drug prices. According to a 2021 study from the RAND Corporation, sick Americans pay on average 256 percent more for medication than people in 32 other Organization for Economic Co-operation and Development, or OECD, countries. When Biden signed the Inflation Reduction Act into law last year, that measure capped out-of-pocket costs for Medicare recipients at $35 per month, but it did nothing for the diabetics who rely on private insurers or have no insurance at all. In August, Senate Democrats attempted to get a $35 insulin price cap passed in their budget package; Republicans blocked the effort.
That Eli Lilly ultimately settled on the same $35 figure that Democrats attempted to pass into law speaks to the enormous political pressure that’s built up around insulin access and affordability. But even if Eli Lilly caps drug prices for insulin in line with public demand, it won’t address some of the systemic reasons that have caused insulin prices to skyrocket. Middlemen, who go between patients and drug companies, have seen their revenue share rise over the last several years. A 2021 study published in JAMA Health Forum revealed that although insulin prices have risen since 2014, the revenue going to the pharma companies has decreased.
The middlemen in question are pharmacies and pharmacy benefit managers, or PBMs, who decide which medications will be covered by insurance companies and with whom drug developers have a strong incentive to strike a good bargain. In 2014, 70 percent of insulin revenue went to pharma companies and 30 percent went to these middlemen. By 2018, only 47 percent of revenue was going to the drug companies and 53 percent was lining the pockets of these opportunistic go-betweens. Rebates that are supposed to be passed on to the patient end up getting pocketed by these entities. Capping the cost of insulin will mean that many insurance companies will be encouraged to make up the revenue elsewhere by charging more for other drugs.
One solution to rising insulin prices hails from California, where Governor Gavin Newsom has proposed establishing a state-owned manufacturing company for generic insulin. The proposal would allow the state to produce and sell insulin at the cost of production, which is roughly $10 compared to the average of $200 listing prices set by pharma companies. According to a paper published by the University of Illinois Urbana-Champaign, the biggest challenge to the proposal is regulatory approval from the Food and Drug Administration to manufacture and sell insulin. However, a state-owned generic drug company could have enormous policy implications. The authors argued that if it were successful, it could address a slew of other pharmaceutical access problems where insurance coverage is limited, such as PrEP—a crucial drug for HIV patients.
So far, the other two major insulin producers, Sanofi and Novo Nordisk, have not announced that they will follow suit and cap their insulin prices. Both drug companies have pointed out that they offer programs of their own to lower insulin prices, such as Novo Nordisk’s MY$99Insulin program, which offers two to three packs of pens for $99 per month. That’s all well and good for many patients, but for diabetics who lack health insurance, a monthly price guarantee from a drug company is not enough to inspire confidence that from one month to the next they will be able to afford the medicine they need to survive.
America is unique in that it believes the burden of health care should be shouldered by individuals rather than society. This creates a severe balance of power issue, in which a pharmaceutical plutocracy sets its own rules and forces patients either to meet those terms or suffer the consequences, all while using its considerable wealth to lobby lawmakers—the better to prevent the passage of legalization that would require drug companies to play by rules set by voters and taxpayers. So let the buyer remember: If Eli Lilly can cap prices today, there is no reason why the company couldn’t have done so years ago and saved the lives of countless individuals who perished because they couldn’t afford insulin. And let the buyer beware: Any prices that Eli Lilly can cap today, there is no guarantee without a federal law in place that it won’t uncap those prices tomorrow.