However much the Build Back Better Act has been whittled down from the Democrats’ $3.5 trillion opening salvo, the latest version still retains some significant goodies, including spending on health care, family leave, and climate. Now that the bill has passed the House, members of Congress and their political allies have been out in force, hyping its contents in order to build public support and encourage the bill’s passage in the Senate, where it can’t afford to lose a single vote.
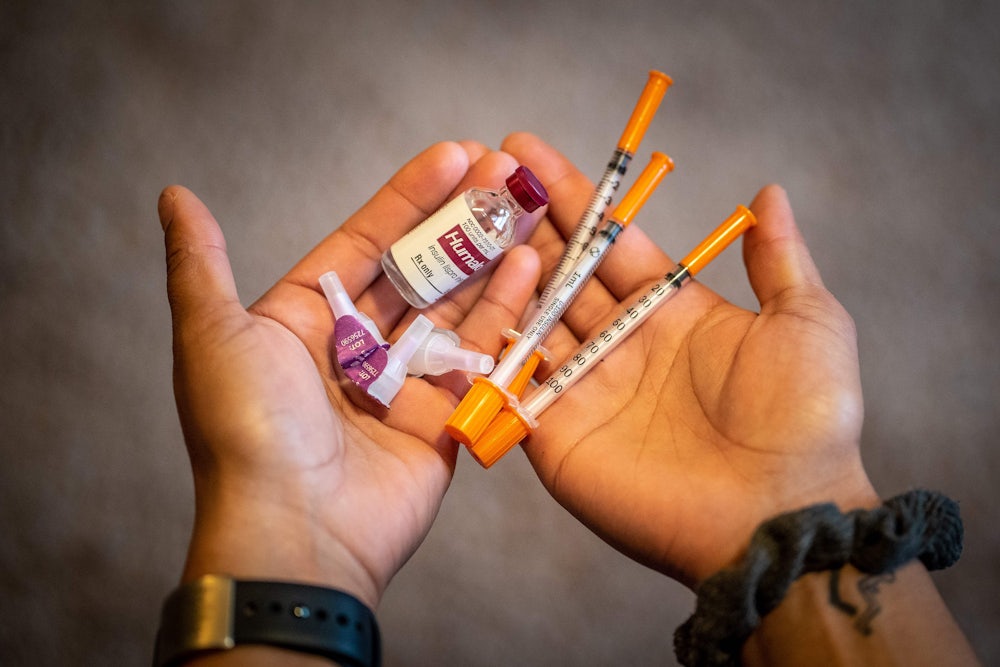
Many of the law’s most ardent cheerleaders have zeroed in on a provision related to a drug whose price has been repeatedly tied to high-profile deaths: “The Build Back Better Act will cap out-of-pocket insulin costs at $35 a month. Thinking of Alec Smith, a Minnesota restaurant manager who tragically passed away because he couldn’t afford the cost of his insulin. This insulin cap is for him and so many others,” tweeted Representative Ilhan Omar. “House Democrats just passed a cap on the price of insulin at $35 a month—and now it’s time for the Senate to get it done,” Senator Ron Wyden blogged at Data for Progress. Even President Biden praised the measure for ensuring “that no one pays more than $35 a month for their insulin.” Dozens more lawmakers echoed these sentiments.
There’s just one problem with this exciting claim about insulin: It isn’t true. Capping the price of insulin would indeed be a seismic achievement, one that diabetes patients have spent years fighting for through grassroots organizing and nonprofit initiatives like T1 International’s #insulin4all campaign. Unfortunately, what’s actually included in the legislation isn’t a price cap at all but rather an insurance copay cap. The deceptively significant difference between the two says everything about how we wound up with a deadly insulin pricing crisis to begin with, and what it will take to stop it.
For years now, Democrats have been running on lowering prescription drug prices—a no-brainer considering how many patients feel the squeeze: The United States notoriously pays more for its drugs than any country on earth, and one poll showed that up to 44 percent of patients report skipping filling their prescriptions because of their high costs. Around 77 percent of Americans think the government ought to do more to make drugs more affordable; even higher numbers support allowing Medicare to negotiate prices down. Anger over high drug prices is perhaps one of the single most unifying issues in a polarized country.
So how did insulin, a drug taken by only seven million Americans, emerge as the poster child for the moral stain of pharmaceutical price gouging? More than a dozen deaths have been directly linked to so-called “insulin rationing” in recent years, including that of Alec Smith—the man Omar mentioned in her tweet. At $300 a vial, short-acting insulin is far from the most expensive drug. It’s not even the only drug whose prices are correlated with higher rates of mortality. But it’s one of many drugs that’s sparked advocacy movements around cost and access issues.
But insulin does serve a uniquely urgent physiological purpose that makes the gazillions of tiny cracks in the U.S. health care system more obvious than any other drug possibly could. For most of us, our pancreases secrete insulin to metabolize sugar on a near-constant basis. Type 1 (and some type 2) diabetics must essentially act as their own pancreas, carefully managing proper doses of prescribed insulin throughout the day—a reality that some patients have described to me as being like doing constant math problems in your head throughout everyday activities.
The health consequences of screwing this up can become dramatic in only a few hours; in less than a day’s time, a mistake or a missed dose can become a medical emergency requiring hospitalization or causing permanent damage or death. While inconsistent dosing or stretches of skipping all sorts of drugs can have dire health consequences, the effects are usually cumulative over time and may be difficult to decisively ascribe solely to drug rationing. But insulin is different: There are very, very few other drugs whose absence can drive such catastrophic effects so quickly and directly.
That makes insulin users intensely vulnerable to all sorts of coverage blips inherent to our health care system. Such gaps can be devastating for anyone—think of what can happen when an uninsured person gets into a car accident. But other minor issues that register as mere annoyances for many patients can be cataclysmic when it comes to insulin—say, realizing that your insurance didn’t go through on a Friday evening or deciding to go two weeks without coverage between jobs. In a system whose functionality hinges on a complicated bureaucracy of profit-driven payers and corporatized providers bickering over bills, there are all sorts of frustrating pitfalls for patients to navigate. Requiring a life-sustaining medication multiple times a day for life inevitably makes it more likely that you’ll trip into one of those pitfalls, at which point you have no choice but to pay full freight. In the years I’ve spent interviewing people with type 1 diabetes, I haven’t met too many who haven’t had to do this at least once.
Those are problems that insulin copay caps can’t solve. Of the known patients who died of insulin rationing over the past several years, most didn’t have insurance at all. While copay caps do help people with high deductibles—or perhaps even change the material calculus of whether insurance is “affordable”—they don’t caulk the many holes in the coverage landscape that make life so dangerous for patients whose survival depends on constant management of their condition. In a system where coverage isn’t universal with the most minimal possible cost-sharing, you simply can’t run drug-pricing relief through the insurance system—however much drug companies may like it. (Unsurprisingly, many state-level insulin copay cap bills were championed by manufacturers.)
In other words, that drug pricing is even a salient political issue at all reflects bad insurance coverage just as much as it does high drug prices. With truly universal coverage, “drug pricing” would hardly be a coherent concept, let alone one that inflames voters. But in the piecemeal system we have, without multiple companies churning out generic short-acting insulins and millions of people saddled with crummy coverage or no coverage at all, the only way to address the root of the insulin pricing crisis is to reduce the list price enough that paying full freight won’t cause emergencies—and it’s inconceivable that drug firms would consider lowering their price to that degree without being forced. Short of systemic overhauls like Medicare for All, the only feasible Option B would be the public manufacturing or government provision of insulin at no cost, as public health departments do for tuberculosis treatment. With only a few million people in the United States on insulin, these moves would hardly be prohibitive! The reason they aren’t on the table, one may reasonably suspect, is it sets a precedent that would expand public intervention in pharmaceutical policy.
So be it! Insulin may crystallize the problems with the U.S. health care system, but it hardly has a monopoly on them. Copay caps will make a meaningful difference for many people. But they can’t help those who are in the most danger. The politics of drug pricing must grapple with coverage, too, and insulin must always be within reach of those without it.