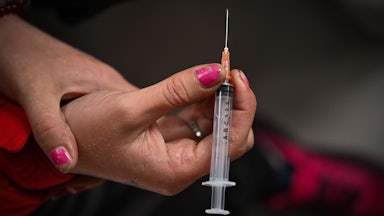
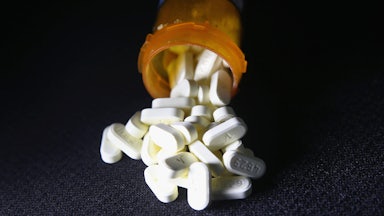
State and local governments have just kicked a major deadline in the disbursement of opioid settlement funds somewhat down the road. Following the combined $26 billion deal with opioid manufacturer Johnson & Johnson and the “big three” distributors this summer, states had the opportunity to opt in to the agreement, and counties and individual towns had until January 2 to decide whether they would receive some of their state’s funds. But the combination of pandemic-related closures and a lack of agreements between states and smaller municipalities slowed the process, and the deadline was extended by a few weeks. States are expected to see money as early as this spring, provided everything falls into place and the complicated business of deciding where funding will actually go is resolved.
The deal, which was reached in July 2021, will disperse a massive amount of cash to states and local governments and could provide an opportunity to mitigate some of the harms done by pharmaceutical companies since the 1990s. But the original settlement was only the beginning of the process, and in the coming months, local governments will have to decide how to offset decades of damage and despair. Just recently, a report from the Centers for Disease Control and Prevention found more than a million Americans have died of an overdose since 1999. Over 100,000 overdose deaths were tallied in 2021. There really isn’t a price tag for numbers like these.
But money is definitely coming, and there will be a lot of it going around: In addition to what’s often referred to as the “global” deal, thousands of individual lawsuits against various pharmaceutical companies will continue to find resolution this year. On December 23, the attorney general of Texas announced the state had reached a $63 million agreement with Endo International,* and in early December, Allergan agreed to pay as much as $200 million to New York state. Fearing a repeat of tobacco company settlements that were spent, for instance, on literacy programs in Colorado and agricultural initiatives in Kentucky, attorneys general have placed some limits on how the money can be spent. The Johnson & Johnson settlement privileges “core abatement strategies” like naloxone and treatment for the incarcerated, though it also allows for funding drug courts and alternative policing models. Notably, neither diversion courts nor criminalization have had much of an impact on overdose deaths, while harm reduction has been shown again and again to reliably keep people alive.
Ultimately, local governments will decide what kind of institutions and programs might have a meaningful impact on the crisis, forming an array of advisory boards and vetting processes to determine what justice looks like in this case. In anticipation of this decision-making process, harm-reduction advocates have begun to lobby for their preferred interventions, asking state governments to fund Narcan programs and medication-assisted treatment. But as one legal expert told Stat News recently, “there is always room in these things for states to perhaps wriggle out of what the original intent was.” In the coming months, these concessions and loopholes will likely become clearer.
There is some reason to be concerned with how opioid settlement money will be spent, if only because of the historical stigma against people struggling with addiction and politicized attitudes toward public health measures like safe injection sites. While attitudes have been shifting slowly, many states are intensely resistant to harm-reduction strategies, balking at the idea of needle exchanges. Last year, Atlantic City voted to close the largest such program in the state. In Louisiana, lawmakers introduced a bill to use their settlement money for drug court; Alabama announced it would take the $9 million from McKinsey & Company—which was found to have helped “turbocharge” opioid sales by consulting for drug companies like Purdue—and use it to fund the district attorney’s office, as well as the state’s forensic science department, to “reduce backlogs resulting from Alabama’s unprecedented volume of opioid-related cases.”
The cognitive dissonance is also on display at the extremely local level. Recently, Mount Caramel, a town with a population of just over 5,000 in Tennessee, held a meeting to decide how it would spend the $150,000 it received from Endo International in November 2021. Among the ideas floated were new police body cameras, donations to a free clinic offering “Christian support” to the uninsured, and $35,000 earmarked for legal services related to eight ethics complaints. These options might be better than Senator Joe Manchin’s 2007 attempt to spend money West Virginia got from an opioid settlement while he ran the state on a $3 million “governor’s helicopter,” but only by a bit.
To prevent scenarios much like this one, several states have formed specific trusts and advisory boards to determine which programs will be funded and keep opioid settlement money separate from more routine municipal budgetary concerns. But in at least one state, the initiative has been slow to get off the ground. As of early December, the 19-person board New York promised to appoint only had one member, an issue that likely had to do with a bureaucratic holdup in the state’s legislature but which made forecasting disbursements impossible, even as officials toured the state to promote all the money they had to spend. Even in a historic moment of reckoning for the companies that manufactured the opioid crisis, how much harm can be undone will be determined by a patchwork of state regulations and by legislative bodies without the greatest track record when it comes to funneling corporate money into the necessary hands.
* This article originally misstated the date and amount of the Texas settlement with Endo International.