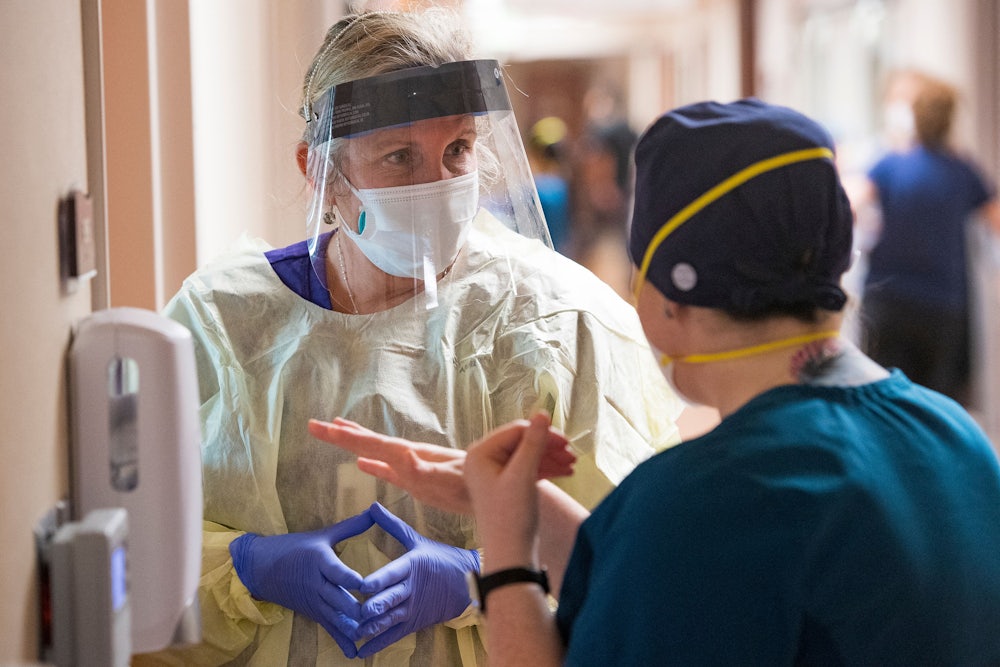
Irene, a nurse working in a Covid-19 unit outside of Boston, has had a lot of jobs since she was licensed in 1998, and she says she’s seen the nursing shortage in action for decades: When she was in her twenties and working in a hospital in New York City, she’d treat as many as 10 patients per shift. Still, this moment feels different. “I know we’re short-staffed,” she said recently, “and I understand people need to get paid.” But she disagrees with the new recommendations that allow for nurses who test positive for Covid-19 to get back on the job more quickly. “Even [the government] said they’re just doing this to keep things running,” she said. It doesn’t inspire a lot of confidence in the Centers for Disease Control and Prevention, the health agency she has looked to for guidance throughout the pandemic, and she feels betrayed by the forces that have conspired to give medical workers looser guidelines rather than higher pay or more staff. “Hospitals have failed us,” she said, “and management has failed us.”
Just prior to the pandemic, Irene (who asked that I not use her full name to avoid retaliation) was a travel nurse in Florida. In late 2020, she returned home to Massachusetts to her kids and took on a series of jobs in addition to her night shift at a small hospital, testing students in schools and then traveling across the state to vaccinate people who were unable to leave their homes. Many of her co-workers have second jobs, she says, and she’s seen people called in to work even when they were sick. When we spoke, Irene had just gotten off an eight-hour overnight shift during which she had to intubate a patient. “I always follow Fauci,” she said. “I trust the CDC. But now it’s every person for themselves, it feels like.” Before we got off the phone, she asked me to make sure I’m wearing an N95 mask when I leave the house.
On December 24, before the CDC altered isolation guidance for all Americans and before government officials impressed on the public the importance of returning to work, the agency issued a series of recommendations designed to offset hospital staffing shortages during a looming wave of infections. Now, nurses are able to return to a health care setting if they are “mildly symptomatic” or asymptomatic after seven days, with isolation times to be cut further should a facility experience a lack of licensed staff. When a health center enters crisis mode—as many hospitals have recently—a nurse who has tested positive for Covid can still show up for a shift, according to a set of contingency plans the agency designed. According to the plan, asymptomatic Covid-positive nurses should be scheduled before those who are visibly sick.
The decision to reduce isolation times for everyone has divided infectious disease experts and dominated the news. But for health care workers, the new guidance has felt like the reflection of a harsh attitude toward a workforce already exhausted and overextended. It didn’t help that around the same time the CDC announced its new guidelines, the Occupational Safety and Health Administration withdrew its emergency protections for health care employers, a program that issued fines to hospitals for failing to follow Covid-19 protocols like logging infections or providing adequate protective equipment. In a moment when it can feel like the government has resigned itself to preventable death, health care workers are being asked to go along with an endless state of uncertainty and brutal working hours that have become the norm over the past two years.
Though some research suggests omicron is a relatively mild variant and vaccines are effective at keeping people who fall ill out of the hospital, on Tuesday the U.S. logged the highest number of positive Covid-19 cases over a single day to date. In California, hospitalizations related to the virus are rising at a faster pace than at any other point during the pandemic. Facilities across the country are entering “crisis mode,” shutting down elective surgeries. And the nursing shortage, which many nurses correlate with a lack of labor protections and low pay, has only deepened as workers seek out higher-paying travel nursing gigs or simply quit.
The latest recommendations follow a harrowing period during which nurses were unable to secure protective equipment, asked to take pay cuts, and worked 12-hour shifts for a months at a time without a day off. “When I first got The New York Times notification I was like, ‘Are you kidding me?’” said Adrianne Kajmowicz, a nurse outside of Chicago. “Everyone else got to stay home” through the pandemic, she said, “and we worked, and this is like a slap in the face.” She’s had three jobs during the coronavirus era, mostly in oncology, so she admits it’s not like she’s going to be caring for many Covid patients in the ICU. But her concerns are existential: “The frustrating thing for me is that I look to the CDC for scientific recommendations, and I have depended on them through the pandemic.… This shows me they aren’t giving us the data; they’re doing policy. They’re saying, ‘Oh, there’s a health care shortage, we need people to work.’”
The day the CDC announced the new guidelines, the National Nurses United union sent a letter to CDC Director Dr. Rochelle P. Walensky disputing the claim that reduced isolation periods would effectively contain the virus: “If the CDC weakens isolation requirements instead of following the science of transmission ... it will lead to increased transmission, illness, and death among nurses, and will worsen the staffing crisis we are experiencing right now,” wrote Zenei Triunfo-Cortez, one of the union’s co-presidents. In an interview, Deborah Burger, also co-president of NNU, said she hadn’t seen such an unpopular policy since workers were told to bring their own protective equipment to work and her Facebook feed was filled with images of nurses wearing bandannas over their mouths. “Nurses understand the principles of infection control,” she said. “It’s their job to prevent the transmission of disease.” But the CDC went “against every single principle” to get medical workers back on the job, she said. She’s highly skeptical of the rule, and she blames poor planning for exacerbating the staffing issues she says preceded the pandemic.
“They want to say that nurses are leaving the profession because of burnout,” Burger said. “That’s nonsense. Burnout implies you’re not doing enough to take care of yourself. It implies the employer has no responsibility. This isn’t burnout, it’s moral injury.” She added that she was amazed there were any nurses left at all.