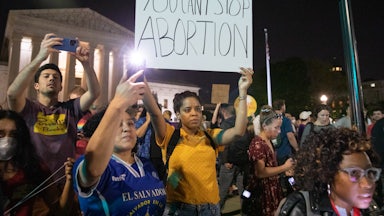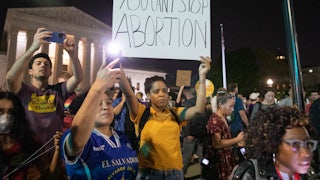Aaron Campbell has known for most of his life that he wanted to be an OB-GYN. When he was 14, in 2005, he dressed up as a doctor for Halloween. It wasn’t a terribly difficult costume to put together, since his father, Morris Campbell, was the medical director at the Knoxville Center for Reproductive Health, now the eastern Tennessee city’s sole independent abortion clinic. Sure, there was that double major in philosophy when Campbell was a student at the University of Tennessee, Knoxville, but he always knew premed would be the final path he’d choose.
As a student, he was a regular presence at the clinic, which is a block north of campus. He would swing by to bring his dad some Boston Kremes from a busy Dunkin’ Donuts that was wedged inside the ground floor of a residence hall. It was on Aaron’s route to the clinic, and the men would share the treats and catch up. During one visit, Campbell saw pregnancy tissue for the first time. “I was already pro-choice at that point,” he said, “but I think if anyone sees something like that, it completes part of an understanding of what really happens.” At that stage in pregnancy when most abortions are performed, at around eight weeks, he added, all you can see is a gestational sac and pregnancy tissue.
Knoxville is currently down to one clinic: KCRH. The Planned Parenthood there was closed after someone set fire to the building this past New Year’s Eve. That it was ruled an arson didn’t come as a surprise; the clinic had previously been shot at in the hours before it opened one day (no one was injured). The other abortion clinic in the region is two hours away in Bristol, but has a cutoff of 14 weeks; KCRH provides care up to 18 weeks. Tennessee’s current law bans abortion at fetal viability, a somewhat fuzzy standard believed to be around 24 weeks. Most of KCRH’s patients are low-income Tennesseans—according to the clinic’s operations director, more than half live at or below the poverty line.

Campbell’s clinic has become a crucial access point for abortion in the Southeast, serving a vast swath of Appalachia that would otherwise lack reliable access. Importantly, KCRH provides abortion care further into pregnancy than any other clinic in the state. These sorts of overloaded access points of abortion care in vast deserts have become increasingly common as states impose further restrictions on reproductive rights. In the months since Texas banned abortion after six weeks, KCRH has felt the ripple effect, taking on patients from as far as Florida who are struggling to get care. If, as expected, the Supreme Court strikes down Roe v. Wade this summer, the country will enter an even more extreme version of this displacement, as hostile states potentially move to ban abortion and decimate these access points.
Dr. Morris Campbell had been an OB-GYN since long before the birth of his son, whom he delivered himself. Soon after Aaron entered the world, he quit delivering babies and shifted the focus of his practice to helping the people who did not want to continue their pregnancy. He also began providing care at the Knoxville Planned Parenthood, and occasionally drove a few hours west to Nashville to help out as well. Once, when Aaron was a boy, father and son went on a road trip. Aaron was in that in-between phase of adolescence where the world begins to come into sharper relief, with all its texture and complexities and mystery. He had started to understand what it was his dad did for work. As a kid in east Tennessee, he sensed the discomfort around the word “abortion” in his community. It dawned on him that his dad’s occupation had led to some precautions that he didn’t see in his friends’ families: living a half-hour away from the clinic, remaining unlisted in the phone book, being told to simply say his dad was a doctor if he was asked by someone unfamiliar. He wanted to know why his dad was an abortion provider.
Morris had probably expected this question from his inquisitive boy, and he told him about what it was like to graduate medical school in 1973, the year the Supreme Court decided Roe. As a student, he saw the damage caused when abortion was outlawed. The lives ruined, the bodies brutalized. He saw women sent away to what he referred to as their “Aunt Sally’s farm” for the summer, clouded in shame, only to return in the autumn with a baby, as if it had magically appeared, as if there had been no blood or pain or mucus, as if life remained unchanged. In sum, Morris “didn’t like the way that women were treated who had an unintended, undesired pregnancy,” Aaron recalled. Upon hearing this, respect settled in his slight chest, and it grew as he did. Aaron has a coat hanger tattooed at the top of his right forearm that he got while he was training to become an OB-GYN in Pittsburgh. Usually, it’s hidden under his shirtsleeve, but it serves as a physical symbol of that conversation and of his father’s legacy.
For a few years, the elder Morris had felt his heartbeat quickening, thumping out unpredictable rhythms in his chest. Then in June 2012, between Aaron’s junior and senior years of college, his father had a fatal hemorrhagic stroke.
After his father’s death, it was clear to Aaron that he needed to accelerate his career. In a state that has put up about as many challenges to abortion as it could, even the loss of one doctor is significant. He dropped the double major to graduate early and move on to medical school at East Tennessee State University in Johnson City, a little more than an hour and a half deeper into Appalachia. As he continued his studies and began rotations, he felt undeniable affirmation that he was on the right track, that this was the thing he could do for the rest of his life to make the world a better place. The determination was important: Abortion stigma runs through the medical field as well, and in a part of the country where culture and religion are inextricable, it can be even more challenging to get the training necessary to provide abortion care.
As a third-year medical student, he ran into trouble when he encountered a patient on his rounds who was 18 weeks and five days into her pregnancy and clearly unhappy about it. “Even in medical school, I never would walk into a room and be like, ‘congratulations,’ because it’s not always a happy thing for people,” he said. “So I would always ask people how they felt about it first.” He asked her if the pregnancy was desired; she told him she didn’t know. “Well, if you want to continue your pregnancy, we’ll be happy to take care of you here,” he said gently. “But if you don’t, the closest place you can go at this point in your pregnancy is Atlanta.” When he made his report to his senior resident, she was displeased that he had presented abortion as an option, and she made her displeasure known in her evaluation of his performance. Though she did not explicitly mention the incident, Aaron is certain that it stemmed from his willingness to discuss abortion with a patient.
A bad evaluation could have wrecked his career before it began and made it nearly impossible for him to be matched with a specialty residency program. Aaron fought the assessment and was eventually given a new evaluation, written instead by his clerkship director, which helped him get into a residency at the Magee-Womens Hospital in Pittsburgh. In his applications, he made it clear that he intended to follow in his father’s footsteps as an abortion provider. After four years, he was finally fully credentialed, and it was time to come home to KCRH. The board of KCRH appointed him medical director in June 2021, the same month he completed his residency in Pennsylvania, and he was back in Knoxville, settling into an apartment near the clinic by the beginning of July.
Less than a year after he returned to his father’s old practice, Campbell is facing the possibility that the clinic may have to shut down, because Republicans in Tennessee have proposed an all-out ban on abortion.
The trouble started in 2020, when the state passed a six-week abortion ban. That law is not in effect; a federal judge blocked it less than an hour after it was signed by Republican Governor Bill Lee, and a federal court affirmed and upheld the stay. It’s been pending appeal for nearly two years.
Last September, a ban on abortions after six weeks went into effect in Texas, and, as of this writing, the Supreme Court has declined multiple times to intervene. Texas’s law has a unique legal spin. Not only is it the most restrictive post-Roe ban on the books so far in the United States, but it also places a bounty on anyone who “aids or abets” an abortion, relies on private citizens to report alleged violations, and empowers them to bring civil lawsuits as a result. The Tennessee Statehouse, as usual, would like the Texas legislature to hold its beer while it offers a comeuppance. In 2022, lawmakers in Tennessee proposed a law under which all abortion is banned. As with the Texas law, there are no exceptions for rape or incest, never mind the mental well-being or the agency of the pregnant person.
For an initial committee hearing on the bill, Campbell put on a purple paisley tie that belonged to his father, carefully combed his hair back, and drove three-and-a-half hours west to Nashville to testify in the House Health Subcommittee in mid-March. On the floor, he spoke in a measured tone, reading from his iPhone well-known statistics that have been heard in this chamber and in many others—that one in four women in the United States will have an abortion in her lifetime, and that complications from abortion are markedly higher in countries where the procedure is heavily restricted. He glanced up intermittently, but he didn’t seem to study the uninterested faces of the lawmakers in the chamber. Reason wouldn’t sway them, nor would emotion. This is well-trod territory. But giving up, not appearing at all, was unthinkable. “Patient safety is paramount, and patient safety will be affected by this bill,” he explained.
Solemnly, Campbell described scenarios in which patients may endure inevitable miscarriage, in which a fetus still has cardiac activity though a miscarriage is well underway, putting the pregnant person at risk of an intrauterine infection, which could lead to sepsis and death. He also referred to nonviable genetic fetal abnormalities. “These are not straightforward issues, and a blanket bill, like this bill, undermines the complexity of health care issues that may be experienced by pregnant women and their physicians,” he told the lawmakers. There were no questions or comments, no response at all to his testimony. The rest of the session was devoted to questions about the legislation, most of which seemed to make the bill’s sponsor, state Representative Rebecca Alexander, uncomfortable. “My intent with this bill is to protect the unborn,” she repeated in lieu of direct answers on the mechanics of the measure. It was approved to send to full committee.
“On one hand, it feels very futile,” Campbell said. “On the other hand, there is that part deep down, that says you need to do the right thing.” Though, ultimately, he added, “they don’t give a shit what I have to say.”
In the end, the legislature pulled the bill from its 2022 session. But that doesn’t take it off the table for the future. The 2020 law to ban abortion after six weeks was also supposedly on ice, but it wound up passing in the middle of the night. And Tennessee is one of 13 states that have a “trigger law” on the books. If the Supreme Court overrules Roe, the Tennessee measure, which was passed in 2019, would automatically make it a felony for doctors in the state to perform any abortions, and would take effect 30 days after the court’s decision.
Campbell knows that his life doesn’t have to be this complicated. “It would be a lot easier somewhere else. But that’s not where people need to be,” he said. “We need to be in states that are hostile to the provision of safe abortion.” Still, he’s put feelers out for work in other states—just in case he soon finds himself with too much time on his hands.